Twenty-year-old Zerina Ahmed was pregnant with her first baby when she arrived with labor pains to Karamile Health Center in Oromia Region, Ethiopia. The midwife on duty, Saada Ahmed, assessed her and informed Zerina that she was in active labor, and would deliver her baby in a few minutes.
In the delivery room, Saada asked Zerina if she would like a companion to be with her during the birth and what position she would like to birth her baby. Accompanied by her mother—who offered her drinks, continuous reassurance, and back massages during labor—Zerina delivered a healthy baby girl.
Karamile Health Center is supported by the Integrated Family Health Program project and MCSP, which aims to reduce maternal, child and newborn morbidity and mortality in USAID intervention sites of Oromia, Amhara, Tigray and Southern Nations Nationalities People. The Program works to increase availability and utilization of high-quality maternal and newborn health services.
Saada, 23, has been working at the health center since July 2014, after realizing her childhood dream of becoming a midwife. She is one of 48 midwives in East Hararghe zone who has received training in Basic Emergency Obstetric and Newborn Care (BEmONC) from MCSP in collaboration with Oromia Regional Health Bureau.
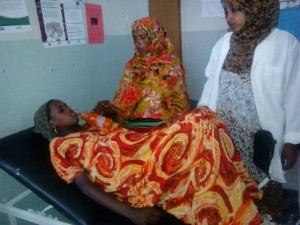
Following the positive management of her labor and birth, Zerina expressed her satisfaction with the care she received: “I am very satisfied with the service I received in this facility from the beginning of my first visit. The midwife treated me politely and allowed my mother to accompany me.”
Zerina decided to deliver at the health center after visiting the facility, at the referral of a health extension worker, for her fourth antenatal care (ANC) appointment.
“My mother’s presence reduced my stress significantly and made me feel comfortable during the labor,” she added. “The midwife called me by name and encouraged me to express my feelings and ask questions.” Zerina was also happy with the coffee ceremony held in the health center to celebrate the occasion, a traditional community ritual when a woman gives birth.
Before the BEmONC training, Saada recalls caring for a woman who she had helped have a normal delivery. When she went to check on her in the postnatal room, the woman was convulsing and unconscious.

“Initially, I panicked and I screamed for help,” Saada said. “But nobody came and it was in the middle of the night. I thought it was a case of epilepsy at first and was not sure how to manage it. Then I sent the guard to call the health officer in charge and the senior midwife while I assessed the mother’s vital signs.”
When help arrived, Saada told them what had happened and they immediately administered magnesium sulphate (parenteral anticonvulsant) and hydralazine (antihypertensive) drugs to bring down her blood pressure. I realized this was a case of eclampsia. After a few minutes, the mother stopped convulsing and recovered.
However, after the BEmONC training, Saada now handles emergency obstetric and newborn cases alone. “I have gained the knowledge and skills and have developed confidence,” she said proudly. “So far, I have successfully conducted three manual removals of placenta, two assisted vaginal deliveries using the vacuum, resuscitated four newborn babies, and administered the parenteral anticonvulsant magnesium sulphate for five mothers with eclampsia.”
Midwives who participated in the BEmONC training have saved a number of mothers, said Bikila Bone, the Primary Health Care Unit Director of Karamile Health Center. This includes patients who have had obstetric complications during pregnancy, childbirth, and the postpartum period.
“This result is reflected in a significant drop of client referrals to a higher level facility and increased client satisfaction,” Bone said, “and has significantly reduced the health officer’s consultation time for obstetric and newborn complications. On top of that, the provision of respectful maternity care after the BEmONC training has increased institutional delivery by 21.45% from April-June 2015 compared to what it was January-March 2015,” Bikila says.

