This content also appeared on JSI’s “The Pump” blog.
Rapid urbanization presents an urgent challenge for the world’s low- and middle-income countries. More than half of world’s population (3.9 billion) now lives in a city; by 2050, this number will skyrocket to 6.3 billion, with 90% of growth occurring in low- and middle-income countries.
An estimated one-third of the urban population (nearly one billion people) lives in poverty. These shifts have created and exacerbated a number of health issues – including the pressing need for immunization strategies and guidelines geared specifically toward urban populations.
Tailoring the Expanded Programme on Immunization service delivery
strategies to fit the context and realities of growing urban immunization inequity will help close this equity gap.
Take the example of Kenya, home to some of the largest informal settlements in the world: while the proportion of Kenyan children who received three doses of DPT (to protect against diphtheria, whooping cough, and tetanus) rose from 86% to 90% between 2009 and 2014, significant inequity in immunization coverage exists. DPT3 coverage in the poorest wealth quintile is 10% lower than in the highest quintile. According to a World Health Organization estimate, in 2013, approximately 353,000 people were unimmunized or under-immunized in Kenya. Moreover, the lowest immunization coverage is found among the children of the poorest households in informal settlements informal settlements, where mothers have low levels of education.

With this in mind, USAID’s flagship Maternal and Child Survival Program (MCSP) conducted a situation analysis in Kisumu City, Kenya to assess the immunization status of children in slum areas, and to understand the challenges and barriers to access and utilization of immunization services among the urban poor. Kisumu City has a well-planned central area with government offices and housing for high- and middle-income residents. Surrounding the central area to the east are the unplanned slum areas, where the bulk of poor migrants settle. The city has 70 health facilities – 20 public and the remainder private, faith-based, or owned by a nongovernmental organization (NGO) – with immunization services provided at 35 (50%) of the facilities.
We found that aggregated facility-level coverage data masks inequity
in immunization coverage in slum areas.
In Kisumu City, immunization services are primarily facility-based and, due to lack of funding, there are no outreach services for slum areas. In addition, the city’s health facilities do not have a strategy to ensure equity in immunization coverage, particularly for the slum population.
And while 2016 data showed high coverage for all vaccines in health facilities, these facilities did not disaggregate immunization data by slum and non-slum areas for monitoring coverage. Moreover, rapid household surveys showed only half of the children in the slum areas of Kisumu City had access to immunization as measured by Pentavalent 1 coverage.
The graph below shows the number of children (12–23 months) MCSP found to be fully, partially, and never vaccinated in Kisumu City slum areas selected for a rapid survey. Access to immunization in these areas is nearly universal, with only two children found to have never received vaccinations; however, many children drop out before completing all immunizations. Overall, 30% – 75% (60% on average) of children in each surveyed slum in Kisumu City began their immunization series, but did not complete their remaining vaccinations.
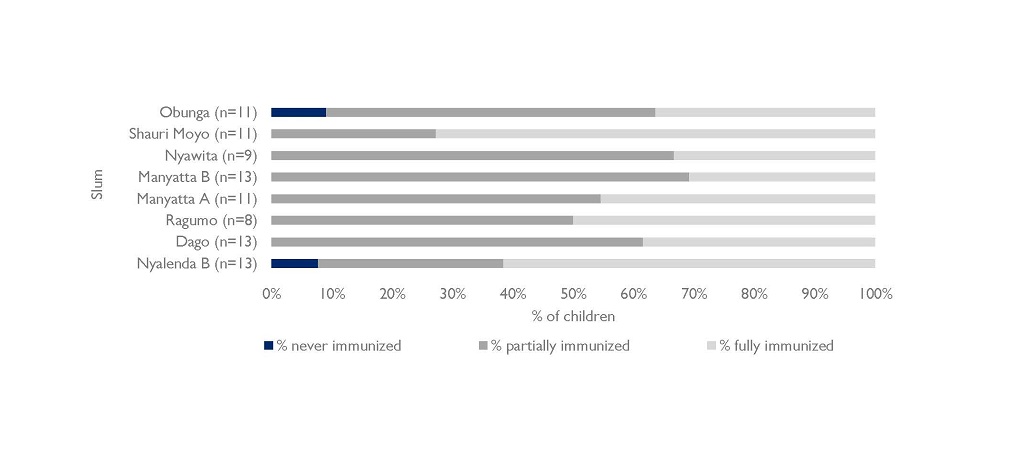
Numerous challenges proved to be obstacles to providing
immunization services to urban poor areas.
Health facility workers named numerous challenges to their provision of immunization services: staff and supply shortages; lack of provider training and funding for outreach; large catchment areas, and frequent migration of people. And because community health volunteers are not paid, most are inactive and unavailable to, for example, follow up with children who missed a vaccine.
Mothers had their own reasons for not being able to fully vaccinate their children. These included “unfriendly” or untrained immunizers at health facilities, and fears of side effects. Others had religious objections or cited competing priorities, such as both parents working outside the home.
“I missed the date to return to the facility for just one day due to a genuine cause, and I feared the nurse will shout on me,” said the mother of a partially immunized child. “So I preferred not to go to the facility due to fear of abusing language of the nurse. Also, I thought she could be rough in giving injection to my child as she is annoyed with me.”
Some simply expressed a lack of motivation – they felt too tired to take their child for vaccinations – while others said their providers did not tell them the date they should return for the next vaccination. Some expressed a fear of HIV testing when visiting the health facility for vaccinations.
That said, other mothers were committed to overcoming barriers and getting their children vaccinated. They understood that vaccines could protect their children from devastating diseases like polio, and that they believed vaccination was their child’s right.
One mother of a fully immunized child said: “A nurse injected my child while talking with another nurse and the vaccine splashed out. The nurse repeated the injection. I felt so bad that I thought I should not return for the subsequent doses, but I went back, as I know the importance of immunization.”
Local leaders in Kisumu City now have the tools necessary to develop a strategy for immunizing the urban poor that is based on an understanding of available resources and outreach activities needed at the facility level. With these tools and more information, leaders can assess their resources and better determine if and how they can extend and improve the quality of immunization services among the urban poor. An important component of the urban immunization strategy is developing a system for tracking infants as they move into, out of, and between slums to ensure that they complete their immunizations.

The first step to meeting the immunization needs of the urban poor is
revealing these obstacles to vaccine access.
Worldwide, immunization averts up to 3 million deaths every year. The World Health Organization estimates that the remaining under-5 deaths — approximately 1.5 million annually — could be prevented with existing vaccines. However, we must expand access to those who need vaccines the most to close these remaining coverage gaps.
While the findings from MCSP’s situation analysis are unique
to the Kisumu City setting, the assessment methodology can be used to do similar immunization assessments in other urban settings.
Successfully reducing or eliminating the spread of vaccine preventable diseases requires reaching every child with immunization. Developing new immunization strategies to reach the world’s large and growing urban poor populations will help to protect some of the most vulnerable children from debilitating and life-threatening disease.
MCSP continues to work with global, regional and national policymakers to develop such strategies, and to promote the Kisumu City assessment as an effective method for gaining an understanding of the immunization needs in an urban poor area and beginning a discussion around reaching and serving the population with immunization services.
To shape our strategy, we must first have the data. This methodology allowed us to map the reality on the ground and clearly identify inequities. Knowing where our efforts are best spent brings us closer to ensuring that every child – regardless of location – is healthy and thriving.

