Buchannan, Liberia – “Look at me at this age, having eight living children,” said Leymah Freeman.* “It’s a serious problem for my husband and I.”
The 35-year-old mother had recently given birth to her ninth and tenth children at Liberia Government Hospital (LGH), a facility whose staff are working with MCSP to address service gaps, provide on-the-job training, and implement new tools to support deliver services and neonatal care.
In Liberia – as in many developing countries – breakdowns in service provision endanger the wellbeing of patients by creating preventable barriers to care. MCSP’s work with LGH aims to reduce the risks to patients like Leymah and her children by promoting service integration before, during and after delivery. The Program is working with LGH staff to identify gaps and barriers to hospital services, and to draw on their own experience to develop workable solutions and improve the quality of care for women and their newborns.
To start, a facility-based Comprehensive Emergency Obstetric and Neonatal Care (CEmONC) and postpartum family planning (PPFP) workshop was conducted at the hospital – rather than in a classroom setting – to allow learners to gain hands-on, practical experience with both models and patients under the guidance of facilitators. It also provided the opportunity to use quality improvement tools to uncover the system breakdowns that were preventing patients from receiving the care they needed – institutional limitations such as equipment problems, unclear staff roles, and missing skills.
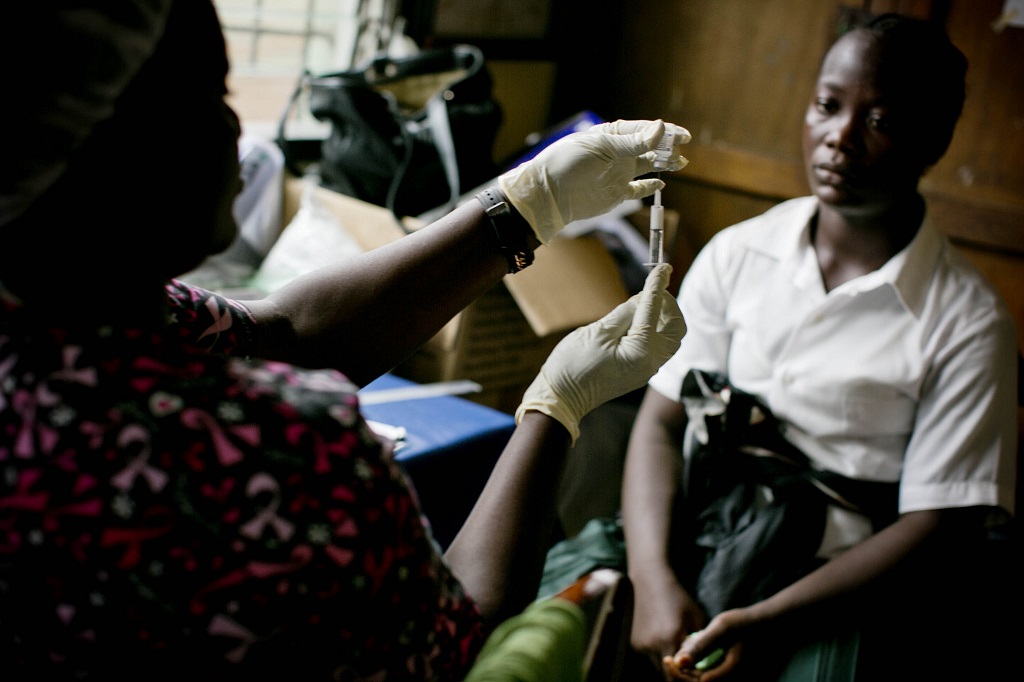
Staff from several hospital departments were invited to participate in the training, with attendees split into two groups that alternated between training modules. One group of health care providers addressed gaps in family planning (FP) provision, particularly for postpartum women. MCSP facilitators discussed techniques for effective FP counseling and demonstrated the insertion and removal of implants and intrauterine devices (IUDs) on models. Because the training was conducted in the hospital, participants were able to practice their new skills –under the facilitators’ close supervision – with real women seeking family planning methods as well as postpartum patients.
The second training group moved through the hospital following a mock scenario with two learners playing the part of a woman in labor and her support partner. As they moved from admissions to the hospital’s service wards, the group learned that the woman was presenting with an obstructed labor and required a Cesarean section. The “patient” had also previously requested an IUD to be placed following delivery.
Moving from triage, to the delivery room, pre-operative room, operating theater, and post-operative room, the staff members critically assessed their service delivery processes, gauged the hospital’s quality of care, noted equipment breakdowns, and discussed solutions. As they did, the facilitators addressed skill gaps with practice on models and patients, helped participants develop process improvement initiatives, and assisted in the creation of action plans to conduct further trainings and replenish equipment.
For instance, during the exercise, the health care providers realized that the hospital suffered from substantial gaps in essential neonatal care. The operating theater and post-operative room lacked a warm area to place newborns who could not immediately join their mothers. In addition, there was no space and insufficient equipment for neonatal resuscitation in both the theater and the delivery room. To resolve these gaps, the hospital staff found a warming lamp under which newborns could be kept in the operating room. They also restructured their delivery room to create space for neonatal resuscitation and developed a plan to do the same in the theater. MCSP continue to work with LGH to ensure that this and other action plans created during the workshop are implemented, providing further support where necessary.
Participants gave overwhelmingly positive feedback after the workshop, including the LGH Medical Director, Dr. Willie-Frank Benson, who said it was the best training he and his staff had ever received. More importantly, the experience moving through their own service delivery process, determining and addressing barriers, and gaining hands-on experience on both models and live patients has led to unprecedented improvements in the hospital’s care of women and newborns.
“[The first time I placed an implant], I very anxious, nervous and sweating,” said Nurse Edith Toe*. “But with support of the MCSP trainers and the LGH FP provider, I inserted this with difficulty, and later I was able to insert the second client’s with ease and smoothly. I felt very happy and want to do more.”
By integrating PPFP and CEmONC services, LGH will be able assist patients in new and better ways, both during and after delivery. For instance, Leymah was able to receive a contraceptive implant immediately after the birth of her twins, which will allow her to choose when she and her husband would like to have another child or to limit the size of their family. This, in turn, will help to ensure that they will have the time, energy, and resources to provide for each of their children as they grow into healthy adults.
“I am so grateful to MCSP and LGH for this counseling and also for training these people to be able to help us,” Leymah said of the care she received. “I will also help to carry this to all of my friends and encourage them to space their children.”