This content originally appeared on the Healthy Newborn Network website.
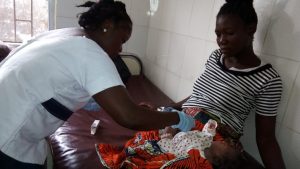
In some parts of the world, an unacceptably high proportion of babies do not survive to 28 days of life due to severe infections that can be prevented through better management of the umbilical cord. Multiple studies have shown that applying the antiseptic chlorhexidine to the umbilical stump shortly after birth is effective in reducing infections. Some studies have even shown a decrease in neonatal mortality. The World Health Organization recommends this simple intervention in high mortality and many home birth settings.
With this recommendation in place, the practice will certainly be adopted in every high-risk setting, right? Unfortunately, no. Successful scale-up of a product or practice is not inevitable. It takes time, sustained financial investment, and active management and coordination for a recommended high impact practice like this to become a widespread component of routine care. Despite its low cost and simple application, chlorhexidine use for umbilical cord care is still rare in many high-risk settings. National health planners may not yet have recommended it as standard practice; chlorhexidine might not yet have made its way into local markets; and health providers and mothers might not be aware of its benefits.
Because new health products and practices like chlorhexidine are unlikely to spread quickly on their own, strategic actions need to be taken to scale them. That is why public health practitioners in countries like Bangladesh, Liberia and Nigeria developed and are implementing national plans to scale-up use of chlorhexidine for umbilical stump care. These plans build on long-term reproductive, maternal, newborn and child health strategies, and set out a detailed roadmap for how key issues specific to scaling up chlorhexidine will be addressed and who will address them.
Scale-up efforts need to be tailored to context. In Bangladesh, a national committee updated national guidelines and training curricula and lobbied for domestic production. In Nigeria, national and state coordinators formed an online community to share stories, advice and encouragement. In Liberia, the Ministry of Health led lesson sharing and coordination among key development partners. When starting the scale-up process, local pilots were helpful in adapting the overall intervention package to the realities of different areas of the country.
“I am happy that this new medicine is here to help us with our babies. During my previous pregnancies, I was always putting… herbs on the navel string for fast action.”
— Mother, Liberia
Various country experiences show that scaling up use of chlorhexidine requires active management by a team of people that have collective influence over important elements of the health system. While the management and partnership structure can be loose, the team still must work systematically to: facilitate scale-up and remove barriers; actively mobilize resources to support scale-up efforts; monitor key information; and make adaptations to plans as needed.
Of note, Bangladesh and Liberia have successfully incorporated a chlorhexidine utilization indicator in the health management information system, facilitating data driven decisions. This is a great improvement over the standard practice during scale up of only tracking outputs that are easier to measure but give less useful information, like the number of people trained or medications purchased. This is like trying to track progress on a car trip by only looking at whether the vehicle has enough fuel and air in the tires, but not actually looking at the road ahead!
To reach the ambitious Sustainable Development Goal targets, it isn’t enough to simply introduce a life-saving intervention. We public health practitioners need to master the art of systematic scale-up if the potential benefits of improved technology, products and practices are to be realized.
To learn more about chlorhexidine in Bangladesh, Liberia, and Nigeria, read the linked briefs.
